As we read this horrifically tragic story, we must ask ourselves, would this happen to a child without an autism diagnosis, would this happen to a child that was blind or deaf? Why is it that the parents of those with the ASD diagnosis are not to be believed when they tell medical professionals that their child’s digestion is not working and that they are in pain? These children have been injured and they deserve compassion and respect.
Patient Safety Awareness Week
Spotlighting Loyola University Medical Center: A Parent’s Perspective
“I need to tell you Alex’s story.” Dorothy Spourdalakis, Alex’s mom spoke professionally with a deliberateness I was not expecting—considering she has been by Alex’s bedside awaiting proper medical care for his gastrointestinal symptoms, for 19 days.
19 days. 456 hours. 27,360 minutes. 1,641,600 seconds.
This is Alex.
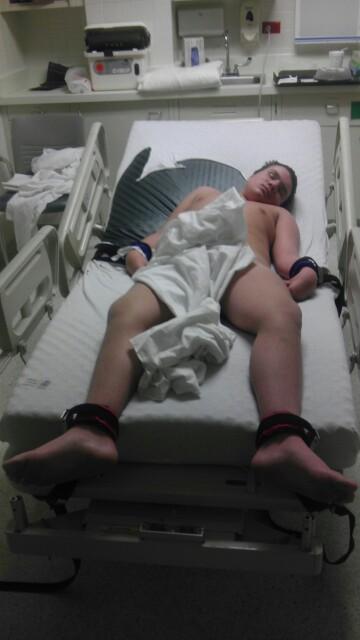 The irony of this week marking The National Patient Safety Foundation’s “Patient Safety Awareness Week” is not lost on Dorothy. According to her, at 14 years of age, Alex has a diagnosis of severe autism and cognitive impairment. He is non-verbal. In October of 2012, Alex began to suffer neurological events that prevented a healthy sleep cycle. He was awake for many hours at a time. Agitation and aggression ensued as a result of sleep deprivation. During this time, symptoms and behaviors that were indicative of severe gastrointestinal distress developed as well. A cycle of constipation, diarrhea and formed bowel movements surfaced and became a chronic problem. On February 16th at 5:00 am, with the assistance of police and paramedics, Dorothy took her inconsolable and highly-distressed non-verbal child to Gottlieb Hospital in Melrose Park, Illinois.
The irony of this week marking The National Patient Safety Foundation’s “Patient Safety Awareness Week” is not lost on Dorothy. According to her, at 14 years of age, Alex has a diagnosis of severe autism and cognitive impairment. He is non-verbal. In October of 2012, Alex began to suffer neurological events that prevented a healthy sleep cycle. He was awake for many hours at a time. Agitation and aggression ensued as a result of sleep deprivation. During this time, symptoms and behaviors that were indicative of severe gastrointestinal distress developed as well. A cycle of constipation, diarrhea and formed bowel movements surfaced and became a chronic problem. On February 16th at 5:00 am, with the assistance of police and paramedics, Dorothy took her inconsolable and highly-distressed non-verbal child to Gottlieb Hospital in Melrose Park, Illinois.
Because of Alex’s physical aggression, he was placed in locked restraints. At that time, Dorothy did not know the ER would be their home for the next several days, as Alex lay naked, in locked restraints, suffering bouts of violent vomiting, severe constipation and diarrhea. Neither she nor Alex bathed for the next 13 days while hospital staff and administrators attempted to devise a plan to care for Alex. “He was given Colace for his constipation and sometimes it would take security staff and nurses more than 15 minutes to arrive to help unshackle him so he could use the bathroom,” Dorothy explained. “Alex would scream as best he could when he knew he was going to have a vomiting episode, but security took several minutes to respond so Alex would lay in his own vomit, waiting to be released by a representative of security. He would be wiped down and returned to the same restraints.”
Autism Is Medical (AIM), a support group that helps parents identify the underlying medical issues associated with the label of autism, was contacted on Sunday, February 24th. They were enrolled to help the staff at Gottlieb understand Alex’s complex medical profile. According to one of the AIM representatives, “Clearly, what they are doing isn’t working.” The AIM advocates,(all mothers to children fully recovered from iatrogenic autism), went on to say, “Currently, this child is being treated with Lorezepam, Oxezepam, Benzatropine, Zyprexa and Ativan. These drugs do nothing to address the intense gastrointestinal issues he is experiencing, nor do they alleviate his pain.” Dorothy explained that Alex remains in a highly-agitated state. He was also prescribed Depakote, to which he had an adverse reaction (elevated lipase). In addition to these issues, Alex’s mom explained he has many allergies. She was told by Gottlieb physicians the standard tests revealing IgE and IgG food allergies were “not reliable and inconclusive.” During his stay in the ER, he ingested milk. When his body reacted, his mother was told it was the bed that caused “contact dermatitis”.
Alex was not assigned to a room at Gottleib and was never formally admitted as a patient. He remained in an ER bay during his entire stay at Gottlieb. He was transferred to Loyola University Medical Center on February 28th at 3:00 p.m. after 13 days in the hopes that they could better serve his needs. It was determined that he needed the care of a pediatric gastroenterologist, neurologist and anesthesiologist, and Loyola could provide those services. On Friday, March 1st, a GI (gastrointestinal) consult was ordered.
Alex and Dorothy were not visited by a gastroenterologist until March 5th, four days after their admission. The physician took an oral medical history on Alex and expressed that he wasn’t sure why they were doing this procedure, and that Alex would be pushed back for some reason having to do with the pediatric anesthesiologist’s “complicated” schedule, according to Dorothy. In the 15 minutes the gastroenterologist spent in the room with Dorothy and her son, an event that was 17 days in the making, he did not see the need to perform a physical exam on Alex.
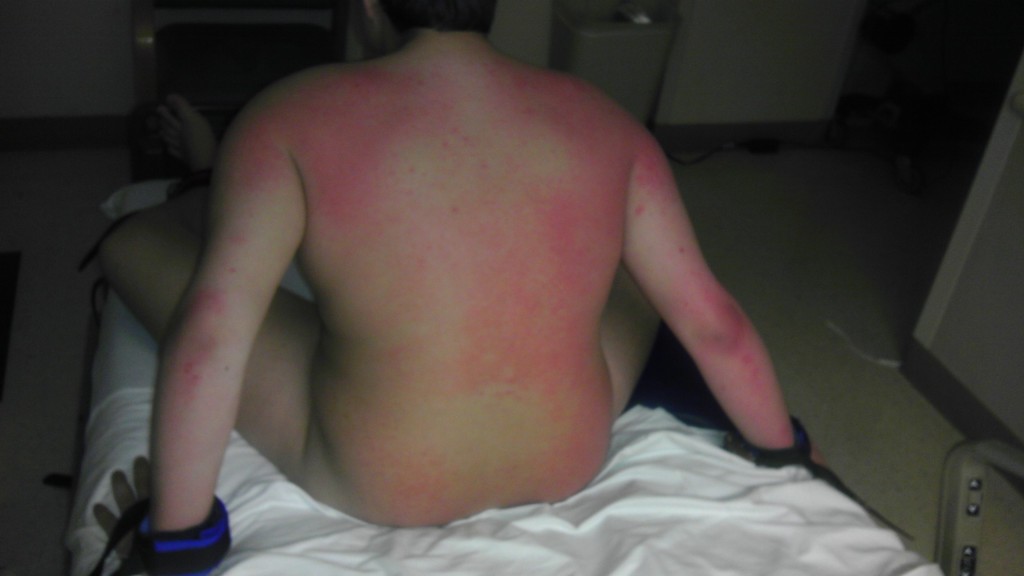 On March 6th, Dorothy met with another gastroenterologist who observed that Alex was indeed in pain. For the first time in 18 days, it was recognized that he was in pain by someone in the hospital system. Dorothy was encouraged. Gastroenterologist number two scheduled the appropriate procedures — procedures AIM founders believe would have been ordered much sooner for a neurotypical child.
On March 6th, Dorothy met with another gastroenterologist who observed that Alex was indeed in pain. For the first time in 18 days, it was recognized that he was in pain by someone in the hospital system. Dorothy was encouraged. Gastroenterologist number two scheduled the appropriate procedures — procedures AIM founders believe would have been ordered much sooner for a neurotypical child.
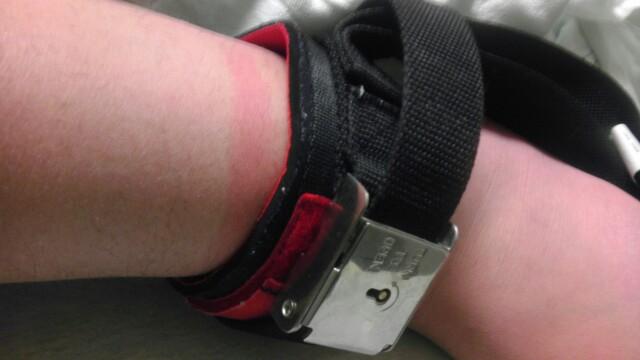
Within hours of meeting with the second gastroenterologist, a CNE (Certified Nurse Executive) spoke with Dorothy and asked to meet with her about insurance issues. During the meeting, she was asked to sign the paper attached below, immediately. Dorothy was hesitant because, “The form is not printed on Loyola letterhead as is the standard policy for routine hospital documentation.” According to Dorothy, during this meeting the CNE admitted the JACHO (Joint Commission on Accreditation of Healthcare Organizations) required assessments of a restrained child by a physician every four hours to reassess his need to remain in locked restraints had not been met. Dorothy said the CNE explained that they may “have missed a few.” (for details on ethical restraint practices please see (http://www.jointcommission.org/)
The same CNE, who previously had promised a plain-clothes security officer for Alex’s room, stated at this meeting there was some confusion on this issue, and he would not be receiving that additional support because it was against hospital policy.
This is the stagnant state Alex has been living in for the past 19 days.
19 days. 456 hours. 27,360 minutes. 1,641,600 seconds.
Alex remains in locked restraints awaiting appropriate medical testing and follow-up care. Dorothy is concerned that no one has given her a plan as to what the exact goals are for his healthcare or how they will be achieved. She is concerned about “weaning” him off the restraints as well. No hospital personnel have addressed this with her. “He has been conditioned to them, now,” she stated.
I asked Dorothy what she wants people to know about what has happened to her son Alex: “I want people to know this is what is happening. They need to know, children with special needs, especially autism, children with cognitive impairments are all at risk for this sort of treatment. All families are at risk. Families who do not speak English, or speak English as a second language are at risk, too. This is how the system is set up. Elderly people are at risk. Who is protecting these children and adults? How can we as a society allow this to happen to our weakest? This is apparently the norm. Their medical needs are met with medications that do nothing to address their physical illnesses but purposefully make them silent and unable to protest any longer. Is this all we have to offer our children, our family members, parents and spouses?” she implored.
The members of AIM confirmed Dorothy’s concerns: “There is no plan for him. Patients who suffer from disabilities are at risk for abuse and neglect. In a day where patient satisfaction scores determine reimbursement rates, and hospitals are competing for market share, I wonder if this same story would unfold if the patient was admitted for heart disease or elective surgery. Policies and safety measures are already in place in every hospital system and acute care facilities across this nation. Internal regulatory audits for things like restraint use, falls and infections are done routinely. Loyola’s website shows pictures of happy patients getting the treatment they need. It highlights partnerships with physicians, a team approach for high-risk pregnancies, their cardiology program — one of the leading in the nation, and the benefit of second
http://www.loyolamedicine.org/Contact Vice President and CNE, Paula Hindel at 708-216-3802 to express your concerns for Alex’s care.Let CEO, Larry M Goldberg know what is happening to voiceless children in Loyola’s healthcare system. 708-216-3215Lisa Joyce Goes is a free-lance essayist, author, Contributing Editor for Age of Autism, and Co-Founder of The Thinking Moms’ Revolution.



Mainstream medicine works for BIG PHARMA ONLY!!! Hospital docs only give medicine, ‘pharmacuetical bandages’ for their medical and physical illnesses. They do not want to find the problems from lab research, only cover the problem up with perscription drugs and snd you on their way! This poor child was experiencing horrible pain and suffering and the only mask the problem instead of finding answers thru lab tests!!! So horrible, immoral, wrong on so many levels….DISGUSTING!!! I am so sorry that Alex had to suffer like this, unreal…….doesn’t any one in that hospital have any morals?!!! SIMPLY OUTRAGEOUS! I WOULD SUE!!!!
People can file a complaint here to assist Alex in getting the appropriate medical care he needs. http://www.jointcommission.org/report_a_complaint.aspx As a parent of a twenty one year old son with autism this was often our fear. Our son has come far with biomedical interventions and coordinated medical care for many years after sustaining a vaccine injury in 1992. But we also know that there are many families that are not so fortunate and need assistance to meet their child’s very specific medical needs. In 1999 my brother, who lived with autism and epilepsy, died in a facility where he was being forcibly restrained both chemically and physically. We need to bring attention to this abuse and stop it once and for all. Thank you very much for running this story.
th,as a nurse for over 30 years
this is an absolute disgrace, I have been a nurse for over 30 years and I cannot understand why even one individual in the health care industry would not have addressed this. my heart breaks for your son and for you ,mom call the media,call your senator call the board of nursing and also the board of physicians for your state……this can not be tolerated………..
Parents of these children need to take control of the health of their children. Dr. Carley can teach parents how, what, when, why. The medical profession is our worst enemy in many ways. Think a minute. They have zero cures. They use only toxic potions. They reject all of the natural and safe cures? They put doctors in jail who cure naturally…. plus many more weird and insane things that should be red flags to parents. Vaccines are a major red flag to many parents and more and more parents are not buying into the lying fear mongering that drives the masses to take toxic potions against every fiber of common sense within. Learn the full scoop about vaccines, learn how to reverse the damage done by vaccines from Autism to cancers to tumors to auto immune disorders…. http://www.drcarley.com
http://www.jointcommission.org/pain_management/
Try him on the GAPS Diet by Dr. Natasha Campbell McBride !! This is awful. Poor Boy
THIS IS JUST SO WRONG.MY GOSH,HE SHOULD BE TREATED SAME AS ANYONE.JUST BECAUSE A CHILD HAS ADISABILITY DOESN’T MAKE THEM ANY DIFFERENT ,THAN ANY OTHER CHILD.HOPING ALEX WILL SOON BE GIVEN THE CARE HE NEEDS AND DESERVES!!
Please send me contact info for this mother, I am an attorney and have an autistic son. This is beyond despicable.
Hi Lester,
I have asked for more info and will come back to you. May I give them your phone number – I think you submitted that to us??
Lester, are you on Facebook?
Thank you for offering to assist. That is what most families need and cannot afford is legal assistance in these cases.
When my daughter was in the hospital for a bone transplant, the girl next to us was a severely handicapped child. She was also in restraints, horribly thin, and full of sores. She was awaiting a new gastronical feed tube so they weren’t feeding her so she wouldn’t aspirate. She kept being put back in the line because for some reason she wasn’t deemed urgent. So this child lay in restraints, unmedicated, not cared for, no comforts, and always crying because that was all she could do. She had a cup of water with a sponge to moisten her lips and that was all…. she would be moving around in pain so blankets would tangle, her only comfort a soft pillow would fall, etc……. as the kind of parent I was, I spent almost every waking moment with my daughter before I went home to my three other children and husband an hour away, every day for a week. I was glad that we could comfort this girl for the 5 days she was there, by moistening her lips, straightening her blankets, and putting on music to soothe her……. for three days before her procedure, we saw nurses maybe twice in the day…… no food, no nutrition, no comfort, her sores weeping, and her soul distraught…… Kiernan would cry and so would I as this poor child suffered. When I asked Kiernan if I should request a move, she emphatically said no, because we were the only people to help this child. I made some very strong complaints about the care in general, and definitely about this poor little girl… no action of course.
Oh my God Kim please, please contact CPS or the joint commission in your state. This is horrific to hear and no child should be left like that. Individuals with disabilities are often left with inappropriate medical care, many are wards of the state and are not provided adequate care. Please do the right thing and not let that child suffer anymore and report the case as soon as possible.
CPS is even worse! They are gov run and do not care about autism!! I’ve heard horror stories from CPS kidnapping autistic kids whos parents try to help them with diet and supps and alternative medicine when main stream medical/docs fail them!
Is there a Chiropractor on board with him? If he is still hospitalized this can be difficult. He needs a professional who understands how to evaluate his nervous system and has the ability to relieve the pressure on his spinal nerves that go to his digestive organs. Is there a way to find a great traditionally trained Chiropractor for him? It would do no harm, and i have seen miracles over and over with this care.
I cannot believe how awful this young guy was treated. There are no valid excuses for this. There are many parties responsible here and they should be held accountable. I hope his parents take this story to the media, and I also hope they seek litigation. These doctors and nurses had the ability and knowledge to provide proper care, they just didn’t make it a priority at all.
This is so wrong on every level. How could so many doctors and nurses see this child being treated so inhumanely and not do anything to ease his suffering?!!?!? This is an absolute outrage. But sadly, the medical model (and big pharma) care more about the $$$$ than they do the actual patients. I am sorry for what your poor son and yourself have endured.
I have a niece who is autistic, also non-verbal. This is a terrifying story. That being said, you waited too long. I would have checked him out after the second day. Contacted his pediatrician. Never would I allow a child of mine to be treated in such a manner.
This is so horrific. i cannot even begin to comprehend this story, as well as Kim Lang’s story. my heart goes out to these parents and children. I do not understand why she cannot get proper doctors in there or transfer him to a facility that knows and understands the issues he has. they are setting themselves up for a big lawsuit. I am sure she is doing everything by the book in case she does take legal recourse, but this is sad. is this how all disabled children/adults are treated in hospitals? if that is the case, we need major change NOW!!!!
Alex Spourdalakis, age 14 is in a room at Loyola Medical Center in Maywood, Illnois outside of Chicago. He has been hospitalized now for over three weeks without appropriate medical care. Three weeks in pain, the majority of that time in four point restraints lying in a bed. This could be my child, your child, but most importantly he is God’s child. He should not be treated this way. Please go to the ireport at the bottom and click on the green button at the bottom that indicates CNN should cover the story. Then post a message if you can. Also sign the petition. Five minute max to assist in saving a life. Share this information please.
Day 19
http://www.ageofautism.com/2013/03/day-19-loyola-chicago-hospital-locks-down-autistic-patient.html
Day 21
http://www.ageofautism.com/2013/03/alex-spourdalakis-loyola-medical-center-ineptitude.html
Day 22
http://www.ageofautism.com/2013/03/day-22-autism-agony-at-loyola-u-medical-center-.html?cid=6a00d8357f3f2969e2017d41cb35c2970c
OCR
http://www.ageofautism.com/2013/03/region-v-chicago-illinois-indiana-michigan-minnesota-ohio-wisconsinceleste-davis-regional-manageroffice-for-civil-r.html
Change dot org
http://www.change.org/petitions/loyola-university-medical-center-give-alex-spourdalakis-the-medical-treatment-he-needs
https://www.change.org/petitions/loyola-medical-center-maywood-chicago-illinois-provide-appropriate-medical-testing-and-medical-treatment-for-alex-spourdalakis
CNN iReport
http://ireport.cnn.com/docs/DOC-942306